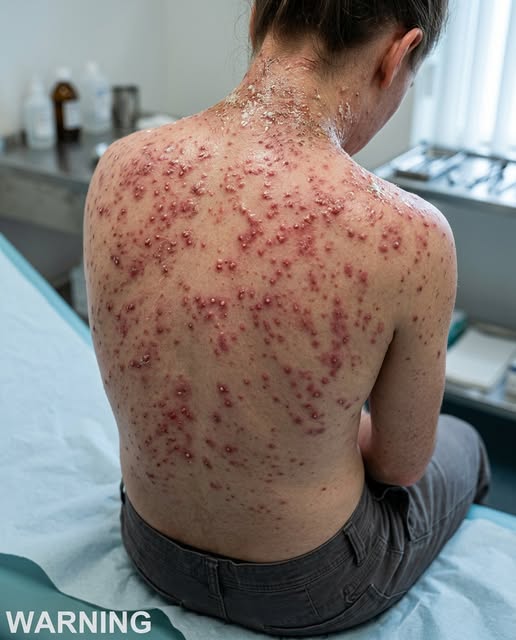
Shingles, medically known as herpes zoster, is a condition that often triggers confusion and concern, largely because many people are unaware of its origins or why it manifests even in seemingly healthy individuals. While it is a relatively common condition, particularly as one ages, understanding the mechanics of the virus is essential for prompt intervention and the prevention of long-term complications.
Shingles is directly linked to the varicella-zoster virus, the same pathogen responsible for chickenpox during childhood. Many people are unaware that once a case of chickenpox resolves, the virus does not leave the body. Instead, it remains dormant for years or even decades, hiding within the nervous system. Under specific physiological conditions, the virus can reactivate, leading to shingles.
This resurgence typically occurs when the immune system is compromised. Factors such as the natural aging process, prolonged stress, chronic illness, immunosuppressive medical treatments, or periods of intense physical and emotional strain can create an environment that allows the virus to awaken. Although it is more prevalent in adults over the age of fifty, it can affect younger individuals if their immune defenses are sufficiently weakened.
A defining characteristic of shingles is that it rarely appears without warning. Initial symptoms are often nonspecific, frequently leading to confusion with other health issues. Patients often experience localized pain, burning sensations, tingling, or hypersensitivity in a specific area of the body. These discomforts may emerge days before any visible signs appear, which can complicate early diagnosis. As the infection progresses, a localized rash typically develops on only one side of the body. This follows a specific nerve path, which explains why the lesions are constrained to a particular area rather than spreading across the entire body. While the physical rash is striking, medical professionals emphasize that the associated nerve pain is often the most intense and persistent symptom.
For most, shingles has a favorable outcome when managed with proper medical care. Antiviral medications, when administered within the first seventy-two hours of symptom onset, can significantly shorten the duration of the illness and lower the risk of complications. When diagnosis is delayed, however, patients face the risk of postherpetic neuralgia—a form of chronic, persistent pain that can endure for months or years after the rash has cleared. This pain frequently causes burning or stabbing sensations that severely disrupt sleep, rest, and daily productivity, impacting both physical health and emotional well-being. Consequently, medical experts urge patients not to minimize early warning signs and to seek professional advice immediately upon suspicion.
Regarding contagion, the answer is nuanced. A person with shingles does not transmit shingles itself, but they can transmit the varicella-zoster virus to individuals who have never had chickenpox or the vaccine. In such cases, the recipient develops chickenpox, not shingles. As a precaution, those with an active outbreak should avoid direct contact with pregnant women, newborns, and immunocompromised individuals.
In recent years, vaccination has emerged as a key preventive strategy. Vaccines are designed to reduce the risk of developing the illness and to mitigate the severity of symptoms if the virus does reactivate. Health organizations strongly recommend these vaccines for older adults and those with known risk factors.
Beyond medicine and vaccines, shingles serves as a reminder that health requires more than just the absence of obvious symptoms. A balanced immune system, effective stress management, and attentiveness to the body’s subtle signals are vital. In many cases, the body provides early warnings long before a condition becomes overt. By understanding the origin of shingles, recognizing its early symptoms, and acting with urgency, one can effectively manage the risks and avoid the unnecessary suffering associated with this complex disease. Being informed does not need to foster alarm; instead, it promotes the vigilance necessary to maintain health and prevent long-term complications.